Periodontitis and general health: why inflammation of the gums is not a local problem

Periodontitis and overall health have a relationship that cannot be ignored. Periodontitis is an infectious and inflammatory disease that affects the supporting tissues of teeth (gum, periodontal ligament, and alveolar bone).
It results from prolonged accumulation of plaque, but the determining factor is not only the presence of bacteria. It is the inflammatory response of the body.
When this response becomes persistent and unregulated, the progressive destruction of supporting tissues begins.
Unlike tooth decay, periodontitis can progress for years with few obvious symptoms. The absence of pain does not mean absence of disease! Now look.
Contents approached
From gingivitis to bone destruction
The process usually starts with gingivitis.
According to the Ordre des Médecins Dentistes (OMD), “gingivitis” is inflammation of the gums resulting from the body’s effort to contain bacterial aggression. These become inflamed, appear swollen and reddened, and may begin to bleed. In gingivitis there is no destruction of the bone or gums, that is, tissues are not affected.”
This reversible inflammation of the gum is characterized by:
- Redness
- Edema
- Bleeding during brushing
If gingivitis is not treated, it can then progress to periodontitis, occurring:
- Formation of periodontal pouches
- Periodontal ligament insertion loss
- Progressive bone resorption
And in this case, the bone loss is irreversible.
For its part, the goal of treatment is to halt progression, not spontaneously regenerate what has been lost.
Low-grade chronic inflammation: the link with overall health
It is easy to notice that active periodontitis keeps the body in a state of low-grade chronic inflammation.
Periodontal bacteria and their by-products can enter the bloodstream through inflamed periodontal sacs.
Simultaneously, the body produces inflammatory mediators such as:
- Interleukins
- C-reactive protein
- Tumor necrosis factors
These mediators do not remain confined to the oral cavity. They circulate systemically and contribute to inflammatory processes in different organs.
- It is here that periodontitis ceases to be only "a problem of the gums".
Periodontitis and cardiovascular risk
Scientific evidence demonstrates association between periodontal disease and:
- Atherosclerosis
- Acute myocardial infarction
- Cerebrovascular accident
Systemic inflammation contributes to endothelial dysfunction and instability of atherosclerotic plaques.
More important is sclerosis: periodontitis is not the only cause of cardiovascular disease. Still, we can assume it as an additional and modifiable inflammatory factor.
Bidirectional relationship with diabetes
The link between periodontitis and diabetes is one of the most studied, as we have seen here. In summary, it is possible to highlight that:
- People with diabetes have a higher risk of developing periodontitis.
- The presence of periodontitis hinders glycemic control.
Periodontal inflammation increases insulin resistance, worsening metabolic control. Periodontal treatment may contribute to improving glycated hemoglobin levels in diabetic patients.
Periodontitis and general health: other associations
While based on this relationship between periodontitis and general health, it is also common to find implications for other pathologies, such as:
- Pregnancy complications
- Respiratory disease
- Worsening of chronic inflammatory diseases
- Although the mechanisms vary, the common denominator is systemic inflammatory load.
Gingival bleeding is not normal and can be a sign
One of the most frequent signs of gingival inflammation is bleeding during brushing.
Should not be attributed to “too strong” brushing. It is a clinical sign of inflammation. Ignoring this symptom allows for silent progression of periodontal disease.
Why is periodontitis still underdiagnosed?
In Portugal, a significant part of the population does not have regular dental consultations.
According to the most recent data from the OMD-promoted oral health barometer 2025, 26% of respondents have only used emergency visits and 2.5% have never seen a dentist.
The most common reasons include:
- No pain
- Devaluation of symptoms
- Delay due to fear or cost
However, this is especially delicate in diseases such as periodontitis which often progresses painlessly into advanced stages.
When tooth mobility or loss occurs, the disease is already in a complex state.
The importance of early diagnosis
In A Clínica we do a careful periodontal assessment that includes, in particular:
- Measurement of periodontal pouches
- Evaluation of bleeding
- Radiographic analysis of the bone structure
With these mechanisms, our experts can act in a personalized way to control bacterial infection; reduce systemic inflammation; stabilize bone loss; and preserve natural teeth.
Periodontal disease control is part of an integrated health approach that uses the latest technology as an indispensable aid.
In fact, the oral cavity is an integral part of the body. Chronic active inflammation, even localized, has systemic repercussions. So, controlling periodontitis is reducing the overall inflammatory load.
Frequently asked questions about periodontitis
The bone destruction caused by periodontitis is irreversible. However, the disease can be controlled and stabilized with proper treatment and periodontal maintenance.
No. Gingival bleeding is usually a sign of inflammation and may indicate gingivitis or periodontal disease.
Periodontitis is associated with various systemic diseases, including cardiovascular disease and diabetes. The relationship occurs mainly through systemic inflammatory processes.
Prevention is based on three pillars:
- adequate oral hygiene
- regular dental appointments
- early diagnosis of gingival inflammation
Most people should have check-ups at least once a year, the frequency may vary according to individual risk.
Periodontitis is a chronic inflammatory disease with an impact on overall health
Certainly it has come to this point and has already cast aside the idea that periodontitis is harmless and that it is only an aesthetic or functional issue.
Gingival bleeding, persistent inflammation or tooth mobility are signs that require clinical evaluation.
Prevention, early diagnosis and follow-up are crucial to preserve teeth and protect global health.
Whenever we talk about oral health, we never tire of remembering that taking care of the gums is taking care of the body.
Schedule a periodontology consultation at A Clínica without further delays and apologies.
You may be interested in:

Movember: taking care of the mouth is taking care of the male body and oral health
Male oral health is linked to heart, energy and even performance. In this Blue November, know why dental care for men is more than aesthetic and is real prevention.

Do you know what Torricado has to do with tooth strengthening? Discover the autumn diet for strong teeth
The autumn diet for strong teeth includes chestnuts, pumpkins and the Cod Pie from Vila Franca de Xira. Here is the dental care in autumn!

When your mouth speaks through your heart: the (silent) relationship between oral disease and stroke risk
The constant headache may not come from the mind, but from the smile. Discover how malocclusion and temporomandibular joint (TMJ) influence well-being.
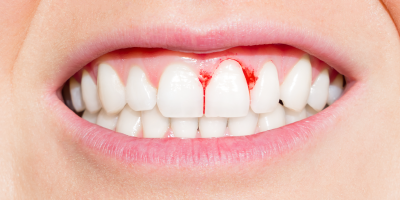
It’s never normal to bleed your gums!
Bleeding from the gums is one of those situations that, although common, cannot be ignored. Take note that at some point, it may even integrate the batch of periodontal diseases, so it is important to know how to avoid such a fact!
